Dr Matthew Cosgrave is a Consultant in Sports and Exercise Medicine. A graduate of Medicine from Queen’s University Belfast in 2011, Dr Cosgrave undertook an MSc in Sports and Exercise Medicine at The University of Bath before completing specialty training in General Practice in Belfast in 2018. Dr Cosgrave worked as a general practitioner with a specialist interest in musculoskeletal and sports team care and as a specialty doctor in pre-hospital medicine before moving to Dublin to complete Higher Specialty Training in Sports and Exercise Medicine in Ireland.
Dr Matthew Cosgrave is a Consultant in Sports and Exercise Medicine. A graduate of Medicine from Queen’s University Belfast in 2011, Dr Cosgrave undertook an MSc in Sports and Exercise Medicine at The University of Bath before completing specialty training in General Practice in Belfast in 2018. Dr Cosgrave worked as a general practitioner with a specialist interest in musculoskeletal and sports team care and as a specialty doctor in pre-hospital medicine before moving to Dublin to complete Higher Specialty Training in Sports and Exercise Medicine in Ireland.
Dr Cosgrave has an extensive background in elite and international sport both as an athlete and as team physician. He has been Team Doctor to The Irish Women’s Rugby Team since 2019 and serves as a Medical Officer to Connacht Rugby Senior Men’s Team. Previous team physician roles include Team Doctor to Team NI at The 2018 Commonwealth Games and 2017 Commonwealth Youth Games, Team Doctor to The Irish Football Association and Medical Officer to The Belfast Giants Ice Hockey Team, Louth GAA, Linfield Football Club and Ulster Rugby Schools.
Dr Cosgrave represented Northern Ireland and Ireland internationally over a 20-year career history in Men’s Artistic Gymnastics, competing at multiple Commonwealth Games, World and European Championships
Hello everybody. My name is Matt Cosgrave; I am a consultant in sport and exercise medicine at the sports medicine department in UPMC SSC. I am delighted to join you this evening to talk to you about foot and ankle issues that affect walking and hiking. Just as a bit of an overview of what we are going to cover today, there is a saying in medicine that common things are common, there are lots of injuries and lots of problems that can happen to the feet and ankle associated with walking and hiking. We are going to look at the main families of injuries, and we will cover some of the common treatment options and the pathophysiology that might be associated with these injuries. We are going to have a look at why we get injured and then we are going to talk in a bit more detail then about how we can prevent these injuries happening rather than focusing on just treating and curing them.
So, what is common? If we think about studies around walking and hiking and the epidemiology of injury one of the biggest studies is from the Appalachian Trails and it looks at respondents from over 1300 hikers over a six-month period. They found that of all hikers who responded 42% of them did not complete their hike with the primary reason being cited as injury. of the of those who got injured, 40% reported foot and ankle injuries as the as the primary issue and this was by far the highest area of injury associated with hiking,13% reported pain in the Achilles tendon specifically and a smaller percentage of only about four reported issues such as stress fractures which we’ll look at in a little bit of detail later. Then there were also walkers and hikers who suffered traumatic injuries such as ankle sprains, and these might have made up about 14% of presentations. Today however our primary focus is going to be looking at some of the overuse injuries that patients get.
So, the first thing we’re going to talk about is plantar fasciitis which is one of the most common presentations of walkers and hikers that attend the clinic here. The plantar fascia is a thick semi elastic band that runs from the heel to the forefoot, its primary job is to help maintain the arch of the foot so when we stand or when we walk gravity and the force of our body wants to push down on that midfoot and it wants to make the arch of the foot collapse, the elastic band then of the planter fascia stretches in a horizontal direction to try and prevent that collapse of the arch. At the heel it is attached at two parts whereas at the forefoot it is attached at five parts at the five heads of the toes and so, for the vast majority of patients the problem tends to occur right at the attachment on the heel. What happens over time is that you get a little bit of micro tearing or micro trauma, if we have the opportunity to rest this then it’ll usually heal. If we do not and we continue to load it continue to walk on it then we tend to develop scarring and a little bit of thickening and stiffening of the tissue. Then what happens is we get a little bit more traction force on the heel and we get a little bit of bruising at the attachment side on the heel. Eventually what can happen is some of those fibres can fail and we can develop some micro tearing at the attachment site, and we call this intra substance tearing. These can be very stubborn and quite difficult to treat.
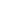
The main way we look at treating these is we look at rehabbing the foot and ankle complex. This is just a bit of a diagram or a schematic of all the muscles and tendons that surround the foot and ankle. I mean if we think about the foot arch itself as it scrolls back round to the inside part of the foot you can see there are a number of muscles within the foot on the under surface that help support that arch. There are also a number of muscles high up in the calf that run down both sides of the ankle and wrap underneath the foot to try and give the foot a side-to-side stability but also help to prop that arch up on the inside. So, when we talk about physiotherapy and rehab for this type of injury really what we’re trying to do is optimise the strength in the muscles within the foot and optimise the strength in the muscles particularly that wrap around the inside part of the ankle and help to support that arch thereby taking away some of the work that the planter fascia has to do. When we struggle with that, we then start to use some other treatment modalities.
This is shockwave therapy, the way shockwave therapy works is it delivers sound waves to the area at a very high frequency. Those sound waves cause the cells to vibrate very quickly. That does two things, one is it stimulates a healing response by mimicking trauma, and the body starts to send growth factors to that area to try and heal. The other thing it does is it desensitises the area, so it can actually function as a little bit of a pain-relieving agent. When we do shock wave treatment we normally recommend starting with three sessions. We would do one session at a one-week interval and after that 3 weeks you should already be starting to see some improvement. I mentioned earlier that some one of the problems with plantar fasciitis is that the connection of the plantar fascia to the heelbone sometimes you are developing a bit of bruising within the heelbone and this is the kind of scenario where shock wave can be very helpful.
In in some other scenarios, we might use injections. The two main injection options that we have are steroid or PRP. We use steroid injections if there’s a lot of inflammation in and around the planter fascia and that’s because steroid acts as an anti-inflammatory it usually has a very quick onset of action and quite often patients feel very comfortable within the first one to two weeks. The downside to it is that it only is a temporary treatment in that it suppresses the inflammation but if we don’t do the other treatment modalities such as the shock wave or the rehab for the foot and ankle to build up the strength around the muscles to support the arch then eventually what will happen is if you go back to walking back to walking a high mileage you’ll be back in the clinic usually somewhere in the region of three to six months later with a recurrence of pain and sometimes even worse because you’ve been walking on under the effects of the steroid and probably causing to some degree a little bit more trauma to the to the planter fascia.
The other option that we have for injection is PRP and that stands for platelet rich plasma. That’s when we take a sample of your own blood from the arm, we spin it in a centrifuge, and we take the platelets from the blood sample, and we inject those directly into the planter fascia. The reason we do this is the platelets have a healing property. They stimulate a healing response and so for all of us we have our planter fascia and our tendons in general they have poor blood supplies. So, what we’re trying to do is take these healing properties that our blood has and put them in a high concentration into the planter fascia to try and stimulate that repair and recovery process. It also has a natural anti-inflammatory effect. The downside to the injection is it can be painful it is also much slower onset of action than the steroid injection and so it may be about six to twelve weeks until you’re really feeling the benefits of it because what it’s doing is it’s stimulating a biological process and we still need to wait for that to happen. The other thing with the PRP injection is because we’re injecting into the planter fascia we’re temporarily causing a little bit of trauma and weakening it and so, we normally recommend that you wear a walking boot for about ten to fourteen days after the injection of PRP which is a little bit more restrictive than some of the other treatment modalities that we have.
If we move on then we’ll look at tendinopathies, the main tendinopathies involve the Achilles tendon which is at the back of the heel. It is the thick rubbery substance that attaches onto the heel, and it attaches the calf down onto the heelbone. We have your tendons that run around the inside of the ankle and support the medial arch. There are three main tendons there is your Tibialis Posterior, your Flexor Halilis longus and your Flexor Doctor and of those three the one that tends to give us the most trouble is your tibialis posterior because it’s the one that hooks around the inside of the ankle and attaches on the midfoot and has the main responsibility of propping up the arch. Then if we go to the outside of the ankle, you have two paranal muscles which stop the ankle from rolling out. So, stop you inverting the ankle or rolling the ankle as an injury and they wrap around the outside of the ankle and attach onto the outside of the foot and then one runs underneath the foot.
What is tendinopathy? I suppose there’s two analogies that we commonly use for this. If we think of a tendon like an elastic its job is to transfer the contractile force of the muscle to the joint and make the joint move. So, if we think about the Achilles or calf muscle contracts it pulls on the elastic that starts to lift the heel off the ground and then the recoil of the elastic is actually what gives you your spring in your step. It’s the same principle for the tendons that run around the inside and the outside of the ankle. The Achilles would just be much more of a power-based tendon, and it would help drive you forwards and drive you uphill. The tendons around the inside and the outside of the ankle, they’re more involved in the control of the side-to-side movement of the foot and ankle. So, if we’re you doing a lot of trail walking where the ground is uneven the tendons around the inside and outside of the ankle are going to have a lot more work to do than if we’re just walking on a on a smooth flat ground.
If we stick to the elastic analogy, what happens with tendons are the same that happens with elastic. If we stretch them nice and gently, they tend to work very well but if we stretch them too much or stretch them too often what happens is they lose some of that elastic property. I suppose that’s to some degree what’s happening within the tendon. Similarly, if we don’t use the elastic or the tendon for a long time what happens is it stiffens up. And then if we go from not using it to so suddenly trying to basket it or try to put a lot of demand on it and we try and stretch it what we tend to find is it’s a little bit resistant to movement and that can often present with pain and inflammation around the tendon if we’ve gone from a period of inactivity to quite a lot of walking or hiking in a short period of time.
What can sometimes happen with tendons as well is if we continue to strain or stress and ignore the signals that the tendon is giving us, we can also develop this intra substance tearing that we talked about within the within the planter fascia. What tends to happen is if we now move to the kind of analogy of spaghetti the tendon is made up of very thin fibres of collagen that are nice and tightly packed together. When we have tendinopathy some of those spaghetti fibres become cooked. Now again the tendon is designed to tolerate tensile force so, if we have dried spaghetti and we pull it from side to side it tends to tolerate that very well. Whereas if we have some cooked spaghetti that’s a bit soft and we pull it from side to side we can split that fibre. So, when we get into a substance tearing of the tendon it’s not torn like a piece of paper, it’s not torn off the bone, what we tend to find is that there’s a little bit of failure of some of the fibres within the tendon and what we’re trying to do in treating it then is either directly treat those torn fibres or we’re trying to treat the fibres around the injured area. So, we’re trying to treat the healthy tendon so that it becomes stronger and it can deal with more of the added burden that’s being placed on.
That takes us then into the treatment modalities and it’s very similar for the Achilles for the for the inside of the ankle tendons and for the outside of the ankle tendons. There’s just a little bit of nuance and specificity in the exercise selection that we use. So some of this might be heel raise activity some of it might involve resisted banded exercises but ultimately it’s a strength-based program that tries to improve the strength in the muscles that are predominantly based up in the calf area and that wrap down around the back of the ankle or the inside or the outside of the ankle. When we’re struggling to get headway with the rehab program we may use shockwave therapy to the tendon or to the tendon attachment site or we may use an injection. Again, if our primary aim is to just suppress the pain so that we can get a good block of rehab we’ll often use steroids. If there’s any damage to the tendon such as intra substance herring, we’ll favour the PRP or platelet rich plasma injection.
So, if we move from the kind of back of the foot and ankle forward to the forefoot there are three main issues that we tend to find with the forefoot. One falls under this umbrella term of metatarsalgia. Now this may involve just some pain and inflammation of the fat pad at the head of our toes, or it may involve something called sesamoiditis which is a very small bone that sits immediately underneath the big toe. Its job is to act as a little bit of a pulley for the for the tendon that runs underneath the foot, and it helps to strengthen the strength and the flexion of the big toe. But what can happen is you can develop some bruising and inflammation both within the bone and around the bone. Similarly, often patients who walk and hike a lot will come in and complain of pain in the big toe itself and that’s because there’s often a lot of movement at the big toe and that movement over time can translate into some arthritis change in the toe. If we move over to the second image what we’re looking at here is what we call a Morton’s neuroma. So, pain in between the toes either presents with pain that we feel in the forefoot or sometimes a numbness and tingling and that numbness and tingling is because a neuroma is essentially a thickening of the nerve that runs between the heads of the toes. Sometimes if we walk a lot or if we wear tight fitting shoes, we can get a bit of compression of that nerve, and it starts to swell and it develops something called a neuroma. That neuroma can simply give us pain, or it can give us some sensory change in disturbance in the food as well.
Moving on to the third image then on the right. What we’re looking at here is essentially what we would see on an MRI of a patient who has a stress fracture or what we call a bone stress injury. When we’re loading the bone, we expect the bone to heal. If we don’t give it the opportunity to heal then what happens is the bone structure starts to break down a little bit. You develop some bruising in the bone structure which is what we see in the image here in the second toe that bright white colour. The beauty of an MRI over something like an X-ray is that often X-rays will miss stress fractures especially in the early stage. And so, MRIs are much more useful and much more sensitive for picking up bone stress injuries and stress fractures.
When we think about treating these types of injuries again they similar they all fall into a fairly similar pattern. If we park stress fractures for a second, I’ll come back to that in a minute, but if we look at metatarsalgia sesamoiditis Morton’s neuroma or something like an intermetatarsal bursitis where we get pain that almost mimics a neuroma but there’s no neuroma present. What we want to do is we want to try and provide as much support around the foot as possible, that’s the first step, something with a stiff forefoot. So, a shoe modification is where we usually start, and a stiff forefoot is something that’s going to give us minimal toe flex. That’s going to allow the force that we translate on the step to almost rock through the bottom of our foot and let us spring off the toes rather than getting a lot of bend or flex in the toe area. If we’re unsuccessful here, we might use some custom fit orthotics. When we think of custom fit orthotics, we can break these into two. We have the lower spec which might be off the shelf that we can mould and there’s a service that we offer here in the clinic where we can look at your foot shape. We can look at the issue that you’re dealing with and then we can mould and fashion what’s effectively an off-the-shelf orthotic to provide a bit more support around your foot that’s specific to you. The higher tech version of this is where you would go in somewhere and you would get something like a 3D scan of your foot and then you would get a bespoke hard orthotic that’s moulded perfectly to your foot size and requirements. The difference between the two is the off-the-shelf version is a little bit more malleable so you can make changes to it more readily. The second benefit is in terms of cost, if you’re thinking about getting something like a custom for fit orthotic you could be paying somewhere from €300 upwards. Whereas something like an off the shelf orthotic can range from €30 to €100. The benefit of getting something like a custom fit or an off the-shelf orthotic with us in the clinic here is that we can tailor the needs specific to you and we can also look at some of the rehab needs of your foot and ankle at the same time as fitting any orthotics.
If we go on, then to look at bone stress injuries in a little bit more detail I just wanted to give you a sense of why bone stress injuries and stress fractures happen. Essentially there’s a constant continue largely between bone healthy bone and bone stress and we know this because there’s been some real great studies done on triathletes who have run for or who have performed in a race and after they’ve raced you’ve scanned them and they’ve had quite prominent bone stress in a number of areas. Now they’re totally asymptomatic of this and after a few days rest and recovery a lot of that bone stress recovers. Now if we know that process is happening when we apply stress to the bone if we don’t get the signals from the bone and we’re not allowing the bone periods of time to rest then eventually what happens is we start to develop a bone stress injury where we start to get pain with it. When you reach that bone stress injury phase the recovery time just takes longer. If we ignore the pain and continue to work, we’ll eventually develop a stress fracture which is a small crack in the bone. It doesn’t necessarily break which is what go which is what happens when we have complete fracture, but it cracks. And again, the implication of that crack is that it just takes much longer to heal. The only way really to treat these is to take away the insult. So, take away the stress that is causing the problem. And for most people that will involve either going into a walking boot for a period of time or depending on the site of the injury it may involve going no weightbearing which might involve using crutches for a period of four to eight weeks depending on the issue.
So why do we get injured? I suppose ultimately it comes down to we are the idea that the demands that we’re placing on the tissue be it the bone the tendon the muscle the planter fascia are exceeding the capacity of the tissue. It can be affected by a number of things; one is just the underlying strength and quality of the bone and tissue. As we age what we tend to find is that the strength and the quality of the tissue reduce. So, age in general, does play a part in this. But these are not all age-related injuries. Despite aging we can often do plenty of work in terms of building up and developing the strength around the tendons the planter fascia the ankle the foot and even the bone that can reduce your risk of injury going forward. Sometimes it can be down to your biomechanics, essentially how you’re moving what way your foot and ankle is shaped and how they move when you plant on the ground and how they move as you walk and hike. Similarly, problems in the foot and ankle can originally stem from issues higher up through the knee or the hip or weaknesses higher up in the knee or the hip because ultimately when we walk there is a kinetic chain that has to do the work to get us from A to B and if we have weaknesses elsewhere in that kinetic chain increased demand and burden can get placed on the foot and ankle.
Training errors is a big issue, I’ll go into that in a little bit more detail, but essentially what training errors refers to is how we approach exercise and activity. How we ramp up that activity or increase it and at what rate we do that and how we approach activity having had a period of downtime. Equipment errors might involve things like footwear old footwear weathered footwear that maybe has lost a bit of its structure and support and then similarly footwear that doesn’t really fit your foot shape or size something with a narrow toe box that’s possibly giving you some metatarsalgia or contributing to Morton neuroma type pain for example. Similarly, we may want to use equipment to help reduce the burden on the feet and ankle and it’s understanding when we need to do that and that might involve something like walking poles or crutches. Under fuelling is a big issue and we see this more and more and it’s something that we’re becoming more and more aware of and essentially what under fuelling refers to is nutrition. So, if we’re going out and exercising especially if we’re going out and doing two to four-to-six-hour hikes or walks are we getting the right nutrition into us to fuel our bodies to fuel our tissues for that walk? And that goes back you know that that’s not just on the day of exercise but how are we approaching it throughout the week in the buildup to that activity? We wouldn’t run a marathon without preparing and often people refer to this as carb loading. There are different versions of this but essentially what we’re trying to do there is we’re trying to provide enough energy and enough fuel for the body to meet its demands, the same thing applies to any activity we do especially longer walks and hikes. Finally, then we think about things like external stressors. You know how busy is life? How well rested and recovered are we? If things are stressful, we’re not getting enough sleep. If we’ve had recent illness or recent injury elsewhere our likelihood of getting injuries in the foot and ankle significantly increase. So, if we think about why we get injured and specifically training error there’s these terrible twos that people often refer to essentially too much activity too soon and too fast.
So too much activity applies to the overall volume. So how many miles how much time we’re spending on our feet and are we is our body prepared to do that. Too soon often refers to our return to activity after having a period off. So, if we think of the spring as being the highest risk period for foot and ankle injuries and for injuries and walkers and hikers that’s because we’ve usually had a period of inactivity over the winter and then all of a sudden, we’ve rapidly wrapped it up when the good weather starts to return and that’s significant. That’s one of the significant issues that people find is that they haven’t given their body enough time to adapt and so their return to activity has been too soon especially after a period off. That’s similar for the too fast, you know we might come back to activity and feel great early on, but we might increase the intensity or the demand too quickly that it may be a case that we go from walking on the flat to terrain or high incline walks in a very short period of time. But that principle is starting slow and giving the body time to adapt over a longer period of time rather than a short period of time and listening to our body for signals, listening to the foot and ankle for any signs or symptoms of pain or stiffness that tells us that we usually need to taper back on things before we can then build on that again.
How do we approach this then? How do we try and reduce the risk of injury? I mean the first thing we’ve got to ask ourselves is what is our baseline? You know are we a seasoned walker or hiker? Is this something we’ve been doing on year on year? Is this something that we’re just wanting to start off a fresh? The more chronic exposure you’ve had in years past usually the better capacity your tissues have to tolerate the demand but then similarly I mentioned it about the spring being the high-risk period what have you been doing over the winter period if you’ve been very sedentary you’re going to need to take things low and very slow at the start and gradually build it up whereas if you’ve been active in other areas such as the gym using other equipment outside of the walking then the likelihood is that you probably don’t need a very long time to adapt and you can usually pick up where you left off or at least get back there within a reasonably short period of time.
What is it that you want to achieve? Are you walking for a specific event that you’re preparing for? And if you are use that as your end point and gradually build yourself up there. Think about it in terms of how much do you want to achieve in a week? How much do you want to achieve in a single walk? It may be a case that you just want to walk 30 minutes a day five days a week and that’s very achievable. But your approach to that should be something like starting off at 10 to 15 minutes a day initially and usually at the early phases of walking we would suggest that you start with an alternate day basis so that you have that opportunity to recover. And once you’re meeting your milestone on an alternate day basis then if you want you can start to introduce that that activity on the day in between. For most walkers and hikers, the weekend is the is the kind of is the milestone and it’s important that we remember that just because we’re doing that one walk on the weekend doesn’t mean that we should do nothing the rest of the week. Because actually if we provide some stimulus to the tissue throughout the week then we’re much less likely to get an injury from the big load that we’re applying to it on the weekend. Whereas if we do very little on the weekend during the week and a lot of the weekend our body struggles to adapt to that in a very short period of time and that’s actually much higher risk of injury keeping things ticking along during the week and then and then just a small jump at the weekend. So just keep that in mind for those of you who like to do your longer two-to-four-hour walks at the weekend.
Then how do you get there? I suppose one is just gradually increasing the vol e and the mileage and think about it in terms of either the distance, the time on feet or the time of the walk but also use things like a pedometer, a watch that might track your steps, and just keep an eye on what your average step count is throughout the week. You can also break it down into days and you can highlight the days where you walk and the days where you maybe do your longer your longer walks. Similarly think about the surface that you’re walking on, If you’re starting off or if you’re just returning flat surfaces are optimum flat and smooth then we might start to introduce an incline and decline and then we can start to introduce some of the rougher more unsteady terrain that’s going to that’s going to put more strain and stress onto the tissues.
So, as a little bit of a summary we want to talk about building volume. So alternate days maybe one longer walk at the weekend start flat then hills then build into terrain and then monitor your load and you should be able to track this fairly easily and when you’re able to track it you’ll be able to see okay ‘is there a day of the week or is there a week that has been a significant outlier to the level of activity I’ve been doing elsewhere?’ , and it often gives you a really good indication and it also gives you a very early sign of where you might have a potential of injury long before any of these problems can happen. I’ll talk to you in a about the 10% rule but that’s something that some patients like to apply if you’re keen on numbers and you want a little bit more detail and to quantify your build of load. The other thing that we think of is our general preparation and this is where the likes of physiotherapy strength and conditioning coaches personal trainers can come in handy and even sometimes if your access to those sort of services is poor there’s lots of options and lots of resources on the likes of YouTube or other social media channels that can help give you a bit of direction around how you should be building up the strength how you should be building up the function and the resilience of your foot and ankle.
At the clinic here our strength and conditioning coaches offer a service that they can look and get some measures of the strength around the foot ankle. They can provide you with an exercise program and they can also provide you with some programming around building up your walking volume especially if you’ve got a targeted goal or event in mind. Nutrition for most people is just a case of making sure that we are getting all our macronutrients a good balance of carbohydrates protein and fat into our diet and making sure that we’ve got good quantities of food that would be enough to fuel our bodies for extended periods of exercise. We do have access to performance and nutritionists, there’s a few that work within the clinic here and if any patients want the direction to those we’d be more than happy to provide that and we can be able to give you a little bit more direction around specific nutritional needs and a bit more education around that. Then finally equipment and that’s thinking about things like footwear orthotics if necessary and then walking such as walking sticks.
Finally, I’m just going to finish on this idea of the 10% rule, and this is largely adapted from running but patients will often use this for patients who are returning from things like stress fractures or from foot and ankle injuries. The basic concept is that we want to reduce our total weekly volume increases by less than 10% week on week. So, if our usual walking volume is one kilometre a week we would want to try and avoid walking more than 1100 meters the following week. Now that’s a very small number but if you extrapolate that one kilometre a week out over five days and we say that we walked 5 kilometres a week over the course of the week we would really want to be keeping our increase the next week to be less than 500 meters in total. As I say it tends to be better for larger volumes and that’s why it tends to be better for those who run but more recently there’s been a little bit of refinement around that advice and there’s been a study that produced in the last year that has found that actually the highest risk of injury occurs in patients who increase a single session activity of more than 10% than any previous walk or hike that they’ve done in the last 30 days. So, for most patients this is the highest risk period in that first month or that first 30 days that you’ve done. If you can gradually build that activity level up to your baseline, then that means you’ve got much more wiggle room in the months ahead where you don’t have to worry too much about small spikes in activity as long as they’re no more than that 10 % increase on your previous longest walk or hike in the last 30 days.
First MTBJ or first big toe arthritis is something that we would very commonly see here at the clinic. I suppose you would start off with standard treatments which would be oral anti-inflammatories. That would be probably kind of the most obvious which you could buy over the counter. If that’s not controlling things for you then you might think about some injection options. First line option injection wise would usually be a steroid injection. We do use PRP injections for these sometimes as well, but the steroid tends to be the first line. It’s got more evidence behind it and usually more effective.
Yeah, the same principle of thought behind them is that they will improve the venus return. So, in order in other words improve the blood flow back up from the extremities to the central system and therefore improve the recovery of the muscle and improve the muscle’s ability to work for longer thereby being able to walk further and more comfortably. So, the same principle would exist for walking as it would for running or any of those other endurance activities. There’s certainly no harm in trying them, how much benefit you would get is sort of person dependent but it’s definitely worth a try.
Well, a LisFranc injury is pretty significant injury. It’s definitely possible. We will treat lots of athletes who’ll get back to high level international sport having had Lisfranc injury. I suppose it’s a little bit difficult for me to comment on that not knowing the full extent of the injury and what was done for it. I would always recommend if you’ve had treatment for it through say a surgeon that you speak to that surgeon for advice on where they feel your level of activity should be. But we would definitely be aiming for getting back to some level of activity and it’s certainly achievable to get back to higher level function with it.
So, the short answer is yes. I thought about talking about this during the talk I suppose when I started training. That was the kind of general advice that we were taught, and it does help. It can definitely improve symptoms; it’s massaging the planter fascia and massaging the tissue around it, and it does provide a little bit of loosening to the tissue, and it allows it to be a bit more pliable. It also desensitizes the area a little so it can make it feel more comfortable but really, it’s a short-term treatment option, you’re treating the symptoms rather than the cause and you may get short-term temporary relief from it. If it’s a case where you walk you massage the food it improves things and you’re able to continue on that on that kind of pathway then that that’s generally fine. But if you’re finding that it’s taking more and more to control the pain or the pain’s not actually going away with it although it’s desensitizing it a little bit then you probably need to be looking at a more definitive treatment option.
So, we rarely tell patients to stop entirely because we do want the foot to continue to work. We want the muscles in the foot and the muscle around the ankle and the calf to work. It really depends on your level of symptoms; we sometimes use a pain score where we say zero is no pain and 10 is agony, can’t put the foot to the floor. We would normally say that something in the region of about 4 out of 10 is a good barometer for where it’s safe to continue. Going above that you’re probably causing more problems than it’s you know than you’re helping. Whereas if you’re below that 4 out of 10 level generally speaking, you’re okay to continue to walk it rather than a kind of walk or not walk. What it’s usually an indicator of is increasing or decreasing the volume or the intensity of your walking. So, as your pain’s reducing you can then start to increase the volume or intensity of your walks. And then the contrary would be as your pain’s increasing you want to be reducing the volume and if you’re getting to a stage where you’re struggling to get out of bed in the morning you’re struggling to put the foot on the floor then really you probably need a period of rest where walking is at a minimum just to allow it to settle down and that it’s that’s not improving things then you need to start thinking about other treatment options.